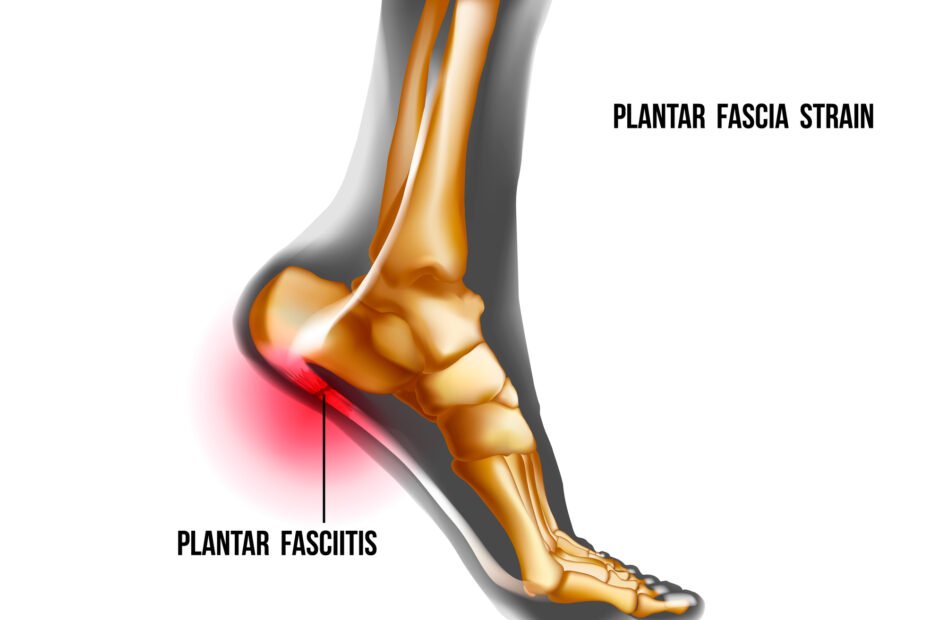
Have you been experiencing heel pain? Does it get worse when you take your first few steps in the morning or after sitting for an extended period of time? You might be suffering from plantar fasciitis. It is one of the most common causes of heel pain, affecting millions of people worldwide. In this blog, we will cover everything you need to know about plantar fasciitis – from understanding its causes and symptoms to identifying the risk factors and getting the right diagnosis. We’ll also dive into non-surgical and surgical treatment options so that you can make an informed decision about your health. Lastly, we’ll address some common misconceptions about this painful foot condition to help clear up any confusion you may have. So sit back, relax, and let’s dive into the world of plantar fasciitis together!
Understanding the Condition
Chronic inflammation and pain result from a common foot injury called plantar fasciitis, often caused by overuse of the tissue in the foot known as the plantar fascia. Identifying the cause and symptoms is essential, as chronic plantar fasciitis can lead to small tears and inflammation in the plantar fascia. The condition usually affects people between 40 and 60 years old, with around 1 in 10 individuals experiencing it at some point in their lives. Diagnosis and treatment are typically provided by primary care doctors.
Definition and Overview
This common foot condition presents as a sharp heel pain, stemming from inflammation in the foot’s plantar fascia. Prolonged standing and flat feet are common culprits of this condition, due to the resultant strain on the lower leg muscles and Achilles tendon. Diagnosis involves medical examination, often followed by physical therapy for treatment. It’s important to address the underlying cause of this condition to prevent its recurrence.

Common Causes
High arches and flat feet often lead to plantar fasciitis. Engaging in physical activities and prolonged standing increases the risk of developing this condition. The continuous pressure on hard surfaces can cause inflammation and foot pain. Repetitive strain and heel bone spurs can result in injury to the plantar fascia. Additionally, tight calf muscles and unsupportive shoes are common contributing factors to the development of this common foot condition.
Identifying the Symptoms of Plantar Fasciitis
Recognizing the symptoms of this painful foot condition is crucial for early treatment. The primary areas of pain are in the arch of your foot and bottom of the heel. Early signs include morning heel pain and stabbing pain in the foot. These symptoms may progress and cause chronic pain over time if ignored, potentially leading to severe cases and nerve damage.
Early Signs
In the early stages of plantar fasciitis, pain occurs in the arch of the foot and bottom of the heel. This is often felt as a stabbing pain, especially in the morning. Small tears in the plantar fascia result in inflammation and foot discomfort. Addressing these early symptoms, such as pain in the front of your foot, is crucial to prevent chronic pain and injury. Proper foot care and supportive shoes can help alleviate the early signs of this condition.
Progression of Symptoms
If left unaddressed, this condition may advance and result in persistent foot discomfort. Chronic plantar fasciitis can lead to long-term pain and walking difficulties, significantly impacting daily activities. Continuous pressure and inflammation can exacerbate the symptoms, potentially causing severe cases. It’s crucial to undergo a physical examination for an accurate diagnosis and to understand the progression of the condition. Ignoring the progression of symptoms can lead to increased discomfort and challenges in mobility.

Risk Factors for Plantar Fasciitis
Risk factors can be attributed to lifestyle and physical factors. Prolonged standing and intense physical activities cause strain on the lower leg muscles, increasing the risk. Flat feet or high arches affect the distribution of pressure on the foot, leading to inflammation. Tight calf muscles due to medical conditions also contribute to the development of plantar fasciitis. Understanding these risk factors is crucial for preventive care and appropriate treatment.
Lifestyle Factors
Long hours of standing and vigorous physical activities can heighten the risk of developing plantar fasciitis. Wearing non-supportive footwear and subjecting the feet to continuous pressure, especially too much pressure, also contribute to this risk. Lifestyle factors such as obesity and sudden weight gain may lead to inflammation and foot pain. Adequate rest and proper, supportive footwear are essential in reducing the risk of plantar fasciitis, making lifestyle modifications crucial for prevention.
Medical Conditions
Medical conditions such as tight calf muscles, flat feet, and high arches can increase the risk of developing plantar fasciitis and foot pain. Chronic plantar fasciitis is often associated with heel bone spurs and inflammation in the foot. Understanding these medical conditions, including the role of the plantar fascia as a band of tissue that supports the arch of the foot, is crucial for effective treatment. Physical therapy and custom orthotics play a significant role in managing the medical conditions related to plantar fasciitis, offering relief and supporting long-term healing.
Diagnosis of Plantar Fasciitis
Diagnosing plantar fasciitis involves a thorough physical examination and assessment of medical history. Imaging tests, like MRI scans, are utilized to determine the cause and severity of the condition. Understanding the symptoms and risk factors is crucial in making an accurate diagnosis. The condition is diagnosed based on symptoms and a physical exam, including a check for inflammation and pain in the plantar fascia. Early diagnosis and treatment are vital in preventing chronic pain and foot injury.

Clinical Examination
During a clinical examination, a doctor will assess the arch, heel, and bottom of the foot, evaluating the plantar fascia and heel bone for tenderness and signs of inflammation. Through this process, the causes of foot pain and discomfort are identified, guiding the development of an effective treatment plan. This evaluation may involve imaging tests, such as MRI scans, to accurately diagnose the severity and cause of plantar fasciitis.
Imaging Tests
Imaging tests are crucial in diagnosing the extent of tissue damage and determining the best treatment approach for plantar fasciitis. X-rays reveal heel spurs and bone abnormalities, while MRI scans provide detailed images of the foot and soft tissue. Ultrasonography visualizes the plantar fascia and inflammation, aiding in assessing the severity of the condition. These tests help healthcare providers understand the cause and extent of the injury, guiding the most effective treatment plan.
Non-Surgical Treatment Options for Plantar Fasciitis
For relief and strength, physical therapy and specific foot exercises can be beneficial. Lifestyle changes and home remedies offer natural relief from symptoms. Supportive shoes and shoe inserts, such as custom orthotics, help in aligning the foot properly. Non-invasive methods reduce inflammation and heel pain effectively. Nonsurgical treatments promote healing and recovery without the need for open surgery. Incorporating these simple treatment methods can significantly alleviate discomfort.

Physical Therapy and Exercises
Incorporating stretching and strengthening exercises for the foot and calf muscles is crucial for recovery. Physical therapy, performed by a trained physical therapist, enhances flexibility and reduces plantar fasciitis pain through tailored exercise regimens. Therapeutic techniques effectively alleviate pressure on the foot, promoting long-term foot care and injury prevention. Additionally, guidance on personalized foot care contributes to individual symptom management and lower leg muscle strengthening.
Home Remedies and Lifestyle Changes
When managing this condition, incorporating rest and ice therapy aids in pain relief and reducing inflammation. Lifestyle adjustments can minimize strain on the foot, while proper foot care and supportive measures are essential for daily activities. Implementing orthotics and shoe modifications improves comfort, and self-care methods effectively manage symptoms, including temporary pain relief. These approaches offer simple treatment methods that can help alleviate discomfort and promote healing.
Surgical Treatments
Understanding the circumstances that lead to surgical intervention is crucial. Exploring the options and techniques used in surgery helps in informed decision-making. Surgical procedures are reserved for severe cases of chronic pain, with risks, benefits, and long-term outcomes carefully considered. Expert evaluation plays a key role in determining the necessity of surgical treatment.
When is Surgery Required?
In cases of chronic, severe plantar fasciitis that does not respond to nonsurgical methods, surgery may be necessary in rare cases. Surgery is indicated when there is persistent pain, limited mobility, and significant foot tissue damage. The decision for surgery is based on the failure of conservative treatments, taking into consideration the patient’s overall health and treatment goals. Collaborative discussions and informed consent are essential for surgical intervention.
What are the Common Misconceptions about Plantar Fasciitis?
Misconceptions surrounding this condition are common. Let’s clarify some of them. From the causes and treatment to foot pain symptoms, there are many myths and misunderstandings. By addressing these misconceptions, we can foster better understanding and provide accurate information on foot health.

What does plantar fasciitis feel like?
It typically causes sharp and stabbing pain in the heel and sole of the foot. The pain is often worse in the morning when taking the first steps, and can increase after prolonged periods of standing or sitting. Some individuals describe it as a dull ache or tightness in the foot after spending a long time on their feet.
Are plantar fasciitis and heel spurs the same thing?
Plantar fasciitis and heel spurs may sound similar, but they are distinct. Plantar fasciitis refers to inflammation of the plantar fascia, while heel spurs are bony growths on the heel bone. Heel spurs can develop as a result of long-term plantar fasciitis. Treatment for both conditions often includes rest, stretching, orthotics, and physical therapy.
How long does it usually take to recover from plantar fasciitis?
Recovery time can vary greatly. While mild cases may resolve within a few weeks with proper treatment and rest, more severe cases may require several months of therapy. Consistent stretching and wearing supportive shoes can help prevent recurrence.
Can it be cured permanently, or is it a chronic condition?
It can be effectively treated, but it may not be permanently cured. Treatment options include rest, stretching, physical therapy, and orthotics. Surgery is rarely necessary and is only considered in severe cases. Proper care and management can help prevent future flare-ups of this common foot condition.

Conclusion
In conclusion, it is important to understand the symptoms and treatment options for plantar fasciitis. Early recognition and intervention can help prevent the progression of symptoms and improve overall outcomes. Non-surgical treatments such as physical therapy, exercises, and lifestyle changes should be considered as the first line of treatment. However, in some cases, surgical intervention may be necessary.
It is also crucial to debunk common misconceptions about this condition, such as the belief that it only affects athletes or that rest alone can cure it. Remember, if you are experiencing any symptoms of this foot condition, consult with a healthcare professional for an accurate diagnosis and appropriate treatment plan.
I hope you found this blog helpful and please feel free to comment and share.
Thanks for reading!
 | Tracy J. Founder, The heel GP |