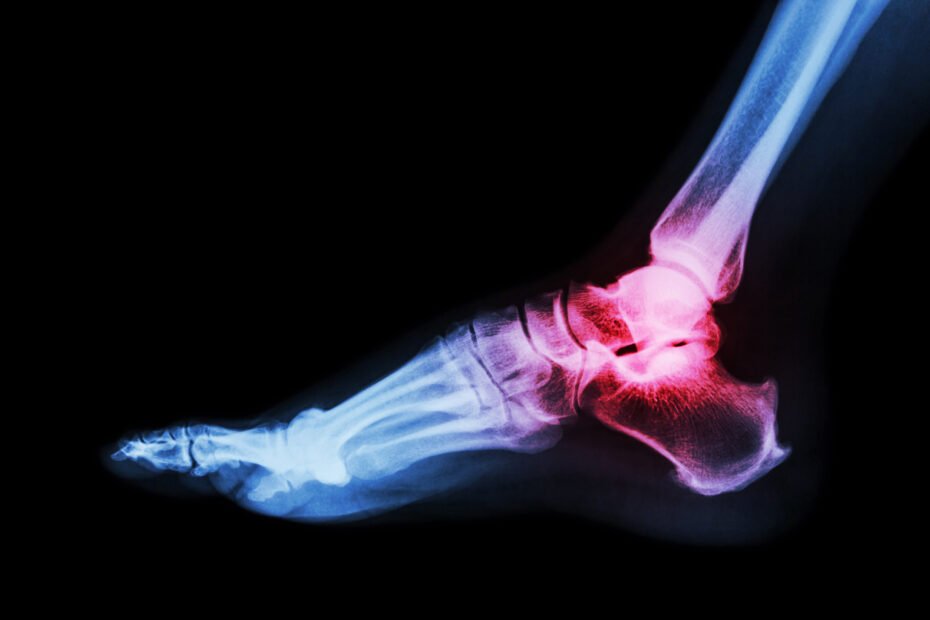
In the quiet hours of the morning, as the world still slumbers, there’s a group of people who wince with each step they take. They know the sharp, stabbing pain in their heels all too well – a reminder of their ongoing battle with plantar fasciitis. This is the story of their journey towards healing, a journey illuminated by the rays of medical imaging, with the focus on plantar fasciitis x ray insights.
Understanding Plantar Fasciitis
Plantar fasciitis, a condition marked by pain in the heel and bottom of the foot, affects approximately 2 million people in the United States annually. It’s particularly prevalent among runners, overweight individuals, and those wearing inadequate footwear. The condition arises from inflammation of the plantar fascia, the thick band of tissue running across the bottom of the foot.
What is Plantar Fasciitis?
Plantar fasciitis is a painful condition that affects the plantar fascia, a ligament-like band of tissue connecting the heel bone to the toes. It is the most common cause of heel pain, accounting for approximately 80% of all cases. The hallmark symptom of plantar fasciitis is intense pain in the heel, usually felt with the first steps in the morning or after periods of rest. This pain can also be triggered by prolonged standing, walking, or physical activity.
The plantar fascia plays a vital role in supporting the arch of the foot and absorbing shock during activities like walking and running. When the plantar fascia becomes inflamed or irritated, it can cause pain and discomfort in the heel. This inflammation is often the result of excessive stress on the plantar fascia, leading to tiny tears in the tissue.
This painful foot condition can occur in anyone, but certain factors can increase the risk of developing the condition. These risk factors include age, with middle-aged individuals being more prone to plantar fasciitis, as well as obesity, foot mechanics, and certain types of exercise or physical activities. Understanding the causes and risk factors of plantar fasciitis can assist in planning the most effective treatment approach for individuals experiencing heel pain.
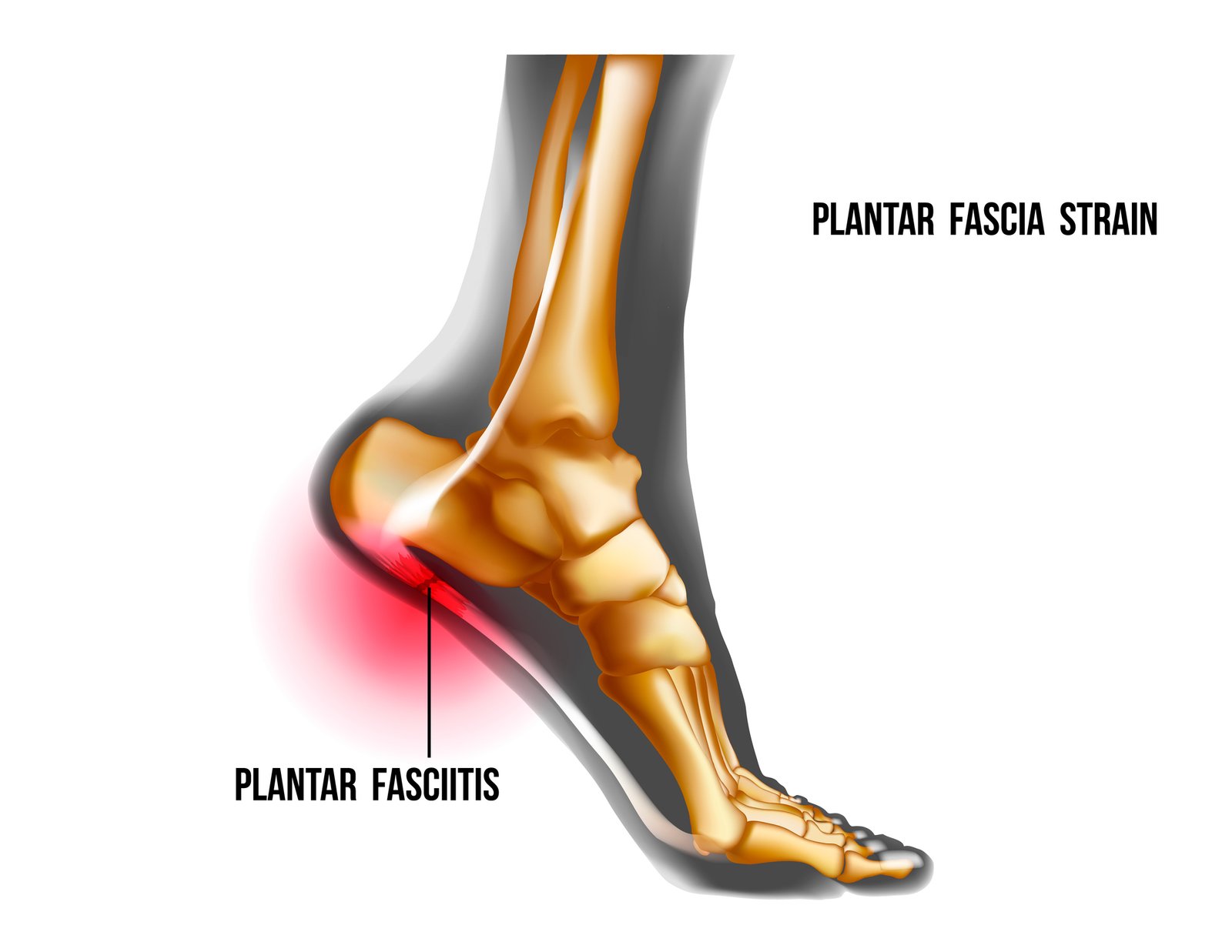
Causes and symptoms of Plantar Fasciitis
Plantar fasciitis can have several causes, many of which contribute to the development of heel pain. Understanding the causes and symptoms of plantar fasciitis can be helpful for accurate diagnosis and effective management of the condition. Here are some key facts about the causes and symptoms of plantar fasciitis:
- Causes of heel pain: Plantar fasciitis can develop due to excessive stress on the plantar fascia, resulting in micro-tears, inflammation, and pain. Common causes of heel pain include:
- Overuse: Engaging in activities that put repetitive stress on the foot, such as running, dancing, or jumping, can increase the risk of developing plantar fasciitis.
- Tight calf muscles: When the calf muscles are tight, they can cause added stress on the plantar fascia, leading to inflammation and pain.
- Unsuitable footwear: Wearing shoes with poor arch support, inadequate cushioning, or an improper fit can strain the plantar fascia and contribute to the development of plantar fasciitis.
- Symptoms of plantar fasciitis: The most common symptom of plantar fasciitis is pain in the heel, typically at the bottom of the foot. Other key features of plantar fasciitis include:
- Tenderness: The affected area of the foot, specifically the bottom of the heel, may feel tender to the touch.
- Stiffness: People with plantar fasciitis often experience stiffness in the foot, especially upon waking up in the morning or after long periods of rest.
- Increased pain with activity: Pain and discomfort may worsen with activities that put pressure on the plantar fascia, such as walking, running, or standing for prolonged periods.
- Risk factors: Certain factors can increase the risk of developing plantar fasciitis, including:
- Age: Plantar fasciitis is more common in individuals between the ages of 40 and 60, although it can occur at any age.
- Obesity: Excess body weight puts additional stress on the plantar fascia, increasing the risk of inflammation and pain.
- Foot mechanics: Flat feet, high arches, or an abnormal gait can contribute to the development of plantar fasciitis.
- Identifying the causes and symptoms of plantar fasciitis is essential for accurate diagnosis and developing an effective treatment plan. By addressing the underlying factors contributing to plantar fasciitis, healthcare professionals can help individuals find relief from heel pain and improve their quality of life.
Diagnosing Plantar Fasciitis
Diagnosing plantar fasciitis involves a comprehensive assessment of an individual’s symptoms, clinical examination, and diagnostic imaging tests. While x-rays do not directly show plantar fasciitis, they play a significant role in ruling out other causes of heel pain and providing valuable information about the foot’s structure. In addition to x-rays, healthcare professionals may also utilize other diagnostic tests such as ultrasound or magnetic resonance imaging (MRI) to confirm the diagnosis of plantar fasciitis and assess the extent of the condition.

The Role of Plantar Fasciitis X Ray
X-ray imaging plays an essential role in the diagnostic process of plantar fasciitis, although it does not directly show the inflamed plantar fascia itself. X-rays are primarily used to rule out other causes of heel pain, such as stress fractures, bone spurs, or calcaneal abnormalities. By comparing the x-ray of a foot with suspected plantar fasciitis to a normal x-ray, healthcare professionals can identify any bone abnormalities that may be contributing to the heel pain.
While x-rays do not diagnose plantar fasciitis, they provide valuable information for accurate diagnosis and treatment planning. They help determine the presence of bone spurs, stress fractures, or degenerative changes in the foot, which can often coexist with plantar fasciitis symptoms. When used in conjunction with clinical history, physical examination, and additional diagnostic tests, x-rays enhance the diagnostic accuracy for plantar fasciitis, helping healthcare professionals provide effective treatment options for individuals suffering from heel pain.
Plantar Fasciitis X Ray Findings
When an x-ray is taken of a foot with plantar fasciitis, the primary focus is on ruling out other bone-related causes of heel pain rather than directly detecting plantar fasciitis itself. However, x-ray imaging can provide valuable findings that contribute to the diagnostic evaluation of plantar fasciitis.
One of the key findings on an x-ray of a foot with plantar fasciitis is the presence of calcaneal spurs, which are bony outgrowths on the heel bone. It is important to note that calcaneal spurs can coexist with plantar fasciitis, but they do not cause the condition. These spurs can be visualized on an x-ray and are often an incidental finding.
X-rays can also help evaluate the thickness of the plantar fascia. In cases of chronic plantar fasciitis or severe inflammation, the plantar fascia may appear thickened on an x-ray. However, it is crucial to keep in mind that x-ray imaging does not directly show the inflammation of the plantar fascia, but rather the associated bone abnormalities.
In addition, x-ray images can provide insights into the overall foot structure, helping healthcare professionals assess bone density, alignment, and the presence of any irregularities in the foot. These findings contribute to the diagnostic evaluation of plantar fasciitis and support the accurate diagnosis of the condition.
Additional Diagnostic Tests
When diagnosing plantar fasciitis, additional diagnostic tests play a crucial role in forming a comprehensive diagnostic approach. Diagnostic ultrasound is effective in visualizing the plantar fascia, assessing for thickness, inflammation, and tears. Similarly, magnetic resonance imaging (MRI) provides detailed soft tissue images, particularly beneficial in complex cases of plantar fasciitis.
These additional tests complement clinical history, physical examination, and other imaging tests, aiding in the correct diagnosis for each patient based on their symptoms and clinical presentation. The choice of the most appropriate diagnostic tests depends on individual patient characteristics and the key features of their condition.
X-Ray vs MRI vs Ultrasound
X-Ray, MRI, and ultrasound are imaging techniques used for diagnosing plantar fasciitis. X-ray shows heel spurs and calcifications, MRI reveals soft tissue damage, while ultrasound displays the thickness of the plantar fascia. Each method has its own advantages in providing essential information for a correct diagnosis. X-ray is useful for osseous causes of pain and to identify the most common site of plantar calcaneal spurs. MRI is considered the gold standard for soft tissue assessment, and ultrasound is helpful in assessing the plantar fat pad, nodules, and bursitis.
Pros and Cons of Each Imaging Technique
When considering imaging techniques for plantar fasciitis, it’s important to weigh the pros and cons of each option. X-rays offer detailed images of bony structures, aiding in bone-related assessments. On the other hand, MRI provides high-resolution soft tissue imaging, allowing visualization of the plantar fascia and surrounding structures. Ultrasound, a dynamic imaging tool, enables real-time assessment of soft tissue abnormalities and inflammation. Assessing the benefits of x-ray, MRI, and ultrasound helps in selecting the most appropriate imaging modality for an accurate diagnosis.
When to Choose X-Ray over Other Imaging Techniques
In clinical diagnosis, x-rays are the gold standard for evaluating osseous causes of pain. They are preferred for bone spurs, stress fractures, and calcaneal abnormalities associated with plantar fasciitis. X-ray imaging is essential in ruling out bone pathologies that may coexist with plantar fasciitis symptoms. Choosing x-ray over other imaging techniques depends on the clinical suspicion of bone-related causes of pain. Understanding the specific indications for x-ray imaging guides the correct diagnosis and treatment approach for plantar fasciitis.
Plantar Fasciitis X Ray Examination Process
During the x-ray examination process, the radiologist will assess the fat pad and look for heel spur, lesions, or nodules on the heel bone (calcaneus) to rule out osseous causes of pain. They will also check the plantar fascia thickness and look for atrophy or ruptures in the plantar fascia. The examination may include an evaluation for tarsal tunnel syndrome, Achilles tendonitis, or other soft tissue abnormalities such as bursitis. This comprehensive assessment aids in the clinical diagnosis and correct management of plantar fasciitis, which is essential for effective treatment.
Preparing for Your X-Ray
Preparing for your foot x-ray involves a few key steps to ensure accurate imaging. Firstly, remove any jewelry or metal objects before the procedure. Additionally, inform the technician if there is a chance of pregnancy. During the x-ray, follow the technician’s instructions on how to position your foot on the x-ray plate for precise imaging. It’s crucial to relax and stay still during the procedure to obtain clear and accurate images without any blurring.
What Happens During an X-Ray?
During an x-ray for plantar fasciitis, the machine emits a controlled amount of radiation to create images. You may need to change positions for multiple angles. The process is painless and takes only a few minutes. A radiologic technologist will guide you, and a radiologist will interpret the images.

Interpreting Your X-Ray Results
When analyzing your x-ray results for plantar fasciitis, several key features should be considered. Look for any abnormalities in the fat pad, calcaneus, or any osseous causes of pain. Pay attention to the plantar fascia thickness and the presence of nodules, which could indicate plantar fibromatosis. Additionally, assess the integrity of the Achilles tendon and look for signs of Achilles tendonitis. Understanding these details can lead to a correct diagnosis and effective treatment plan.
How to Read an X-Ray for Plantar Fasciitis
When examining an x-ray for plantar fasciitis, it’s crucial to identify abnormalities like bone spurs, calcifications, or stress fractures. Pay close attention to the heel bone, plantar fascia, and the foot’s soft tissue. Assess bone density, alignment, and any irregularities. Understanding x-ray images helps identify the underlying causes of pain. For an accurate interpretation, consult a healthcare professional. This knowledge aids in making a correct diagnosis and implementing the most effective treatment plan.
Understanding Medical Terms Used in X-Ray Reports
Understanding the terminology used in x-ray reports is crucial for comprehending the diagnosis. Medical terms such as calcaneal spurs, fasciitis, and inflammation may indicate specific conditions affecting the foot. Additionally, terms like stress fractures, bone density, and soft tissue abnormalities provide valuable insights into potential foot pathologies. Familiarity with these terms related to foot anatomy and pathological features is essential for accurate interpretation of x-ray reports by healthcare professionals. Seeking clarification on any unfamiliar medical jargon or terminology mentioned in x-ray reports is integral to understanding the diagnosis.
Treatment Options for Plantar Fasciitis
Plantar fasciitis treatment options involve various approaches to alleviate pain and promote healing. Non-surgical treatments include rest, ice, compression, and elevation (RICE), along with physical therapy and custom orthotics to support the foot’s arch. Corticosteroid injections can provide temporary relief, while extracorporeal shock wave therapy may stimulate healing. In severe cases, surgical intervention may be considered, such as plantar fascia release. The choice of treatment depends on the severity of symptoms and individual patient needs, emphasizing the importance of a personalized approach.
Non-Surgical Treatments
When addressing plantar fasciitis, non-surgical options are often the first line of treatment. Rest, ice, stretching, and supportive footwear can provide relief, while physical therapy, custom orthotics, and night splints aid in pain alleviation and foot support. Non-invasive treatments such as injections, shock wave therapy, and ultrasound therapy target the underlying causes of heel pain without invasive procedures, focusing on improving mobility, reducing inflammation, and promoting tissue healing. These methods offer patients a way to address their condition without the need for surgery or more invasive interventions.
Surgical Interventions
Surgical interventions for plantar fasciitis may involve releasing the plantar fascia ligament. Procedures like endoscopic plantar fasciotomy or fascia release aim to alleviate chronic heel pain. Surgical options are considered for cases where conservative treatments have not provided relief. The goal of surgical interventions is to address the root cause of plantar fasciitis and restore foot function. Recovery and rehabilitation play a vital role in the success of surgical interventions for plantar fasciitis.
Living with Plantar Fasciitis
Living with plantar fasciitis can be challenging due to constant foot pain, especially during the first steps in the morning. It’s important to manage pain through proper footwear and orthotics. Additionally, stretching exercises and physical therapy can help alleviate discomfort. Understanding the importance of rest and avoiding activities that exacerbate the condition is crucial for effective management.
Home Remedies and Self-Care Tips
Alleviate plantar fasciitis pain with stretching exercises, supportive shoe inserts, and ice application to reduce inflammation and pain. Resting the foot and avoiding exacerbating activities are crucial for recovery. Over-the-counter pain relievers can manage discomfort. Consider the fat pad, achilles tendon, heel spur, and tarsal tunnel syndrome for a clinical diagnosis. A systematic review may identify plantar calcaneal spurs as the most common cause of heel pain in the general population. Utilize sonography and CT for radiology assessment.
Lifestyle Changes for Managing Plantar Fasciitis
To manage plantar fasciitis, maintaining a healthy weight is crucial for reducing pressure on the plantar fascia and easing symptoms. Supportive footwear, especially during physical activities, can prevent further aggravation. Avoiding prolonged standing or walking periods is necessary for effective management. Utilizing orthotic devices provides extra arch support, relieving strain on the plantar fascia. Lastly, engaging in low-impact exercises like swimming or cycling helps maintain overall fitness without adding stress to the foot.

Can Plantar Fasciitis be Prevented?
Preventing plantar fasciitis is possible with regular stretching of the calf muscles and plantar fascia. Gradually increasing physical activity intensity, wearing appropriate footwear, maintaining a healthy body weight, and engaging in lower limb strengthening exercises can also help prevent this condition.
Can you see plantar fasciitis on X ray?
Plantar fasciitis cannot be visualized on an X-ray, but it can help rule out other causes of heel pain. Additional tests like MRI or ultrasound may be needed for a confirmed diagnosis. Treatment often involves stretching, rest, and physical therapy.
Can an X-ray detect other foot problems that may be causing my heel pain besides plantar fasciitis?
An X-ray can identify other potential sources of heel pain, such as fractures or bone spurs, apart from plantar fasciitis. However, it may not always reveal soft tissue damage that could contribute to the pain. In some cases, additional imaging tests like an MRI might be needed for a comprehensive diagnosis. Consult a healthcare professional for accurate assessment and treatment of foot pain.
Is an X-ray a painful procedure for someone with plantar fasciitis?
Getting an X-ray for plantar fasciitis is a non-invasive procedure that doesn’t cause pain. It helps diagnose the extent of damage to the plantar fascia. The X-ray technician will guide you through the process and position your foot on the machine for the image. If you feel discomfort, inform the technician immediately.
How long does it take to get the results of an X-ray for plantar fasciitis and what do they tell you?
X-ray results for plantar fasciitis are typically available within a few days. These results can reveal the presence of bone spurs or fractures that may be causing the pain. However, it’s important to note that X-rays alone cannot diagnose plantar fasciitis, as it is primarily an inflammation of the foot’s tissue. Additional imaging tests like ultrasound or MRI may be required for an accurate diagnosis.
Once diagnosed with plantar fasciitis, how often are X-rays necessary to monitor the condition’s progress?
X-rays are not always required to monitor the progress of plantar fasciitis. They are typically ordered if there is suspicion of a bone fracture or underlying condition. Instead, doctors may use physical exams and other imaging tests like ultrasound or MRI to track the condition’s development. The frequency of follow-up appointments and tests will depend on the severity of the condition and the treatment plan.

Conclusion – Plantar Fasciitis X Ray
Recovery from plantar fasciitis varies, with many experiencing relief within a few months to a year. It’s crucial to adhere to the prescribed treatment regimen and modify activities to avoid aggravating the condition.
As we journey through the narratives of those afflicted by plantar fasciitis, it’s clear that understanding and treating this condition goes beyond just an x-ray. It’s about a tailored approach to therapy, the right support, and most importantly, the resilience of the human spirit.
For more information and support on your journey to recovery, visit theheelgp.com, where a wealth of resources awaits.
As you embark on your journey to recovery, have you considered how an X-ray could illuminate your path to a pain-free life?
I hope you found this blog helpful and please feel free to comment and share.
Thanks for reading!
 | Tracy J. Founder, The heel GP |